Identifying potential hospice patients and coordinating your team
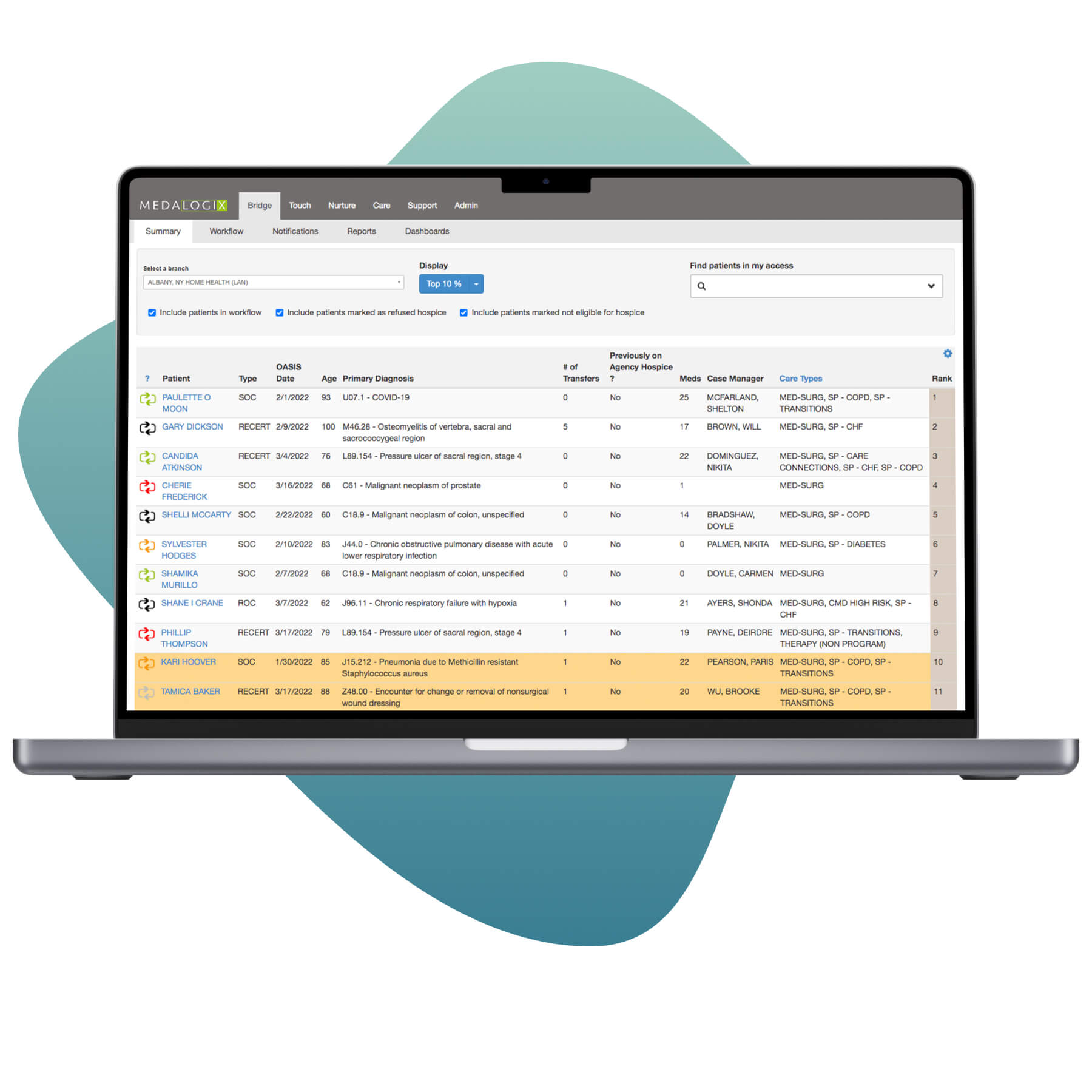
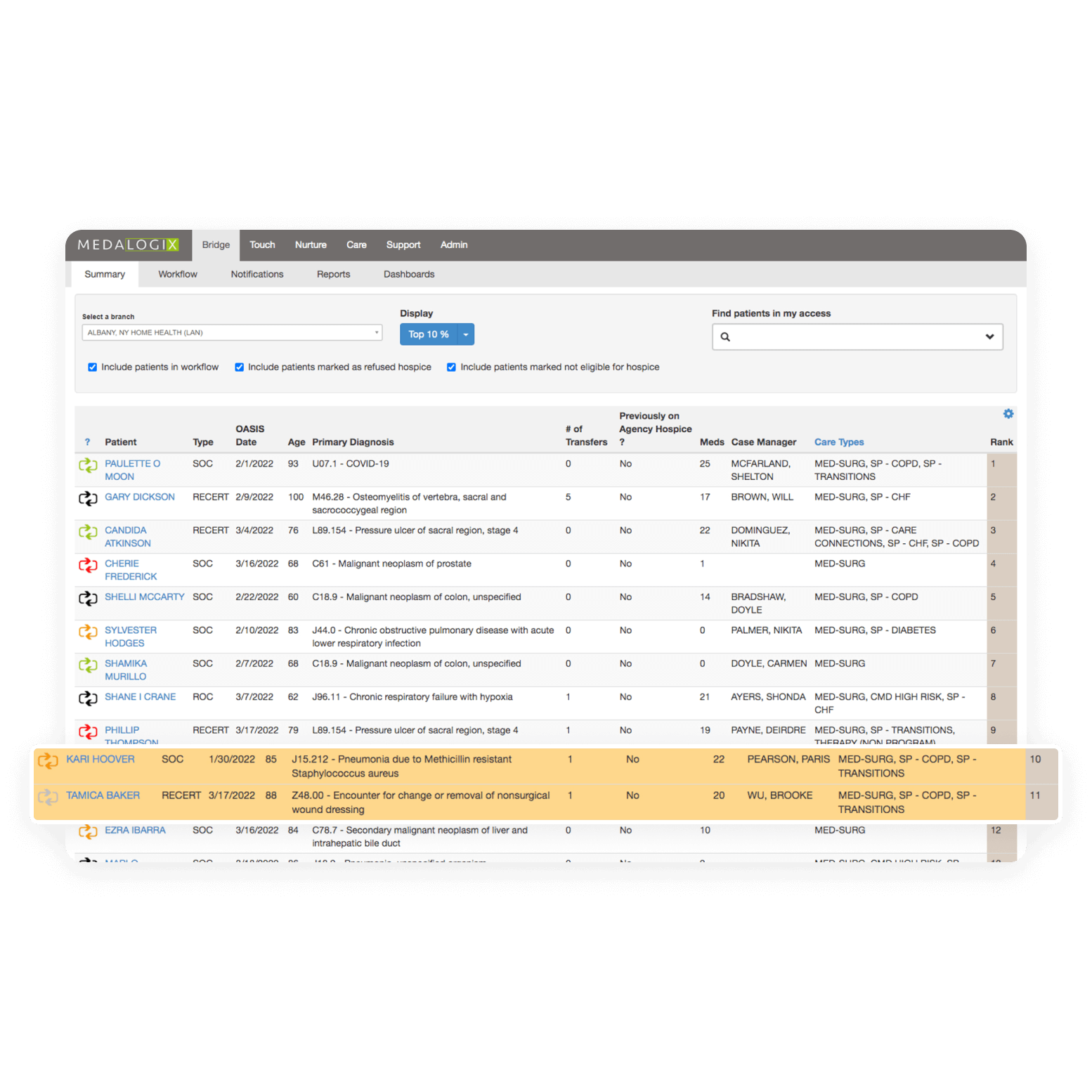
A 2021 study from the Stanford School of Medicine found that although 80% of Americans say they would prefer to die at home, only 20% do. Medalogix Bridge supports patients’ wishes, using machine learning to identify patients earlier who are most likely to benefit from hospice. This leads to dramatic improvements in care quality and efficiency.